GOSH patient first in the UK to receive improved kidney transplant
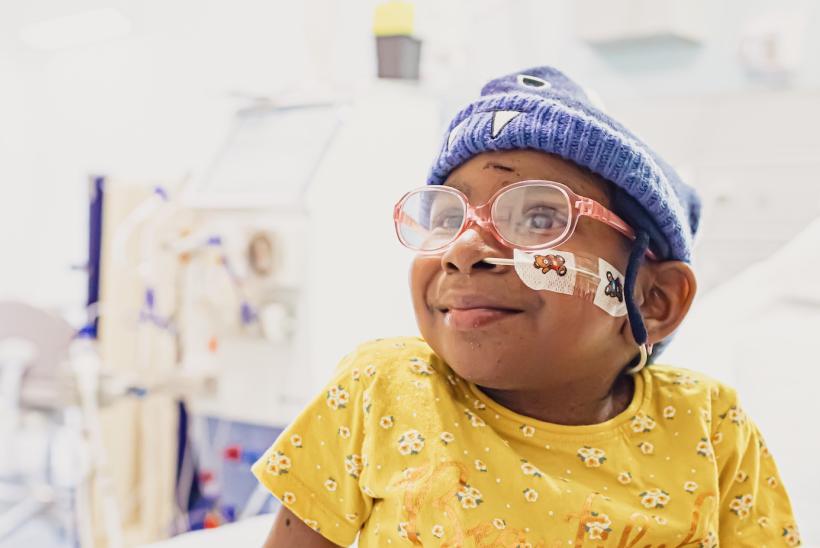
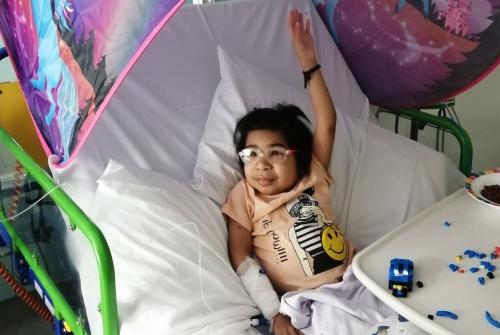
Eight-year-old Aditi is the first child in the UK and on the NHS to be taken off immunosuppressants just one-month after kidney transplant at Great Ormond Street Hospital (GOSH).
This is only possible because Aditi had an immune condition for which she received her mother’s bone marrow six months before receiving a kidney transplant for severe irreversible kidney failure. This reprogrammed her immune system to be the same as her donor kidney, so her organ would not attack Aditi’s body.
Multiple teams at Great Ormond Street and UCL GOS ICH worked together for many, many months to make this possible., including the Bone Marrow Transplant, Paediatric Intensive Care, Immunology, Nephrology, Surgical, Anaesthesia and Renal Transplantation teams.
A life-changing double transplant
Aditi’s life has been transformed. With her double transplant she has gone from being on haemodialysis in hospital three days a week, to being full of energy. Aditi is now back at home and enjoying singing, dancing and playing on her scooter.
Usually, organ transplant recipients are on immunosuppressant medications for the life of their kidney transplant. As Aditi is not on these medications, she is able to avoid their side-effects, including increased risk of infection – therefore reducing hospital admissions and complications after a kidney transplant.
"We were told very clearly; transplant wasn’t the right option."
Aditi has immune and irreversible kidney failure. She was first referred to GOSH when she was five years old, and by March 2021 her kidney function dropped drastically.
A genetic test revealed the cause of Aditi’s symptoms – she has Schimke’s immuno-osseous dysplasia – a rare genetic condition that affects one in one to three million children in the UK.
Uday, Aditi’s dad, said: “We were told very clearly; transplant wasn’t the right option. If she had a kidney transplant, it would be harmful because her own immune system is so low, the donor organ would be more powerful than her body and attack it.”
Dialysis was the only option for Aditi.
Uday said: “This was a big change and an emotional set back as we had only heard what dialysis means - to be stuck on a machine for days."
Team collaboration
While on dialysis, multiple teams at Great Ormond Street and UCL GOS ICH, including the Bone Marrow Transplant, Paediatric Intensive Care, Immunology, Nephrology, Surgical, Anaesthesia and Renal Transplantation teams with international colleagues to deliver the best possible treatment plan for Aditi. This involved a bone marrow transplant to help her immune system gain strength, so that she would then tolerate a kidney transplant from her mother, who was a suitable match.
Uday said: “We were so glad to see other children stepping out of Eagle ward and getting better, but for us it was difficult knowing that Aditi's bone marrow transplant was imminent. This was so scary as you know that your child will have chemotherapy and lose their hair and become poorly.”
For four weeks Aditi was on the intensive care unit having her bone marrow transplant, whilst having continuous dialysis for 24 hours a day, every day.
Uday said: “The team came down from Robin (bone marrow transplant) ward and let us turn on the machine to deliver her transplant, or “my mum’s new cells” as Aditi says.
“Aditi was different to other children on the intensive care ward, as she was so upbeat and chatty. She would be singing, and that is how the nurses remember her, and we remember each of them for their outstanding care.”
"We take our organs for granted, but we all have such a gift in us."
Six months later in March 2023, Aditi was well enough to have her kidney transplant.
Uday said: “A week before the transplant, Aditi went to Guy’s Hospital and visited her mum’s transplant team. On the day itself I raced between Guy’s and GOSH to be with Divya and Aditi. Every half hour I was receiving calls updating me on Aditi’s and her mum’s progress.
“The past three years Aditi’s energy had been lost to dialysis. After her kidney transplant, almost instantly, we saw such a big change in her energy levels.
“We take our organs for granted, but we all have such a gift in us.”
Just one month after her kidney transplant, Aditi was able to be taken off immunosuppressants as her immune system saw her new kidney as its own.
Now back at home, Aditi is thriving. She looks after her new kidney incredibly well, referring to it as a flower that needs water to bloom, much like her plants that she enjoys watching grow.
Uday said: “The past three years she has been restricted with a Hickman line [a tube which delivers treatments and take blood samples directly from a vein] and all she wanted to do was for her line to go away so she could go and splash in the water. She is now starting swimming lessons.”
“Aditi is always dancing and singing, and the first to put her hands up for anything musical. We are so happy that she can excel and be the amazing version of herself that she is, thanks to her dual transplant.”
"This is the first time I have cared for someone in 25 years who has not required immunosuppression after kidney transplantation."
Usually, if you have a kidney transplant you are on immunosuppressive medications for the rest the life of the transplanted organ to reduce the risk of the body rejecting the new, unfamiliar, organ. The continued use of these drugs has many side effects including infections, high blood pressure and even kidney damage.
Using the same donor for the bone marrow and kidney transplant means that the immune system is reprogrammed so that it becomes a match for the new kidney – reducing the problems associated with rejection as much as possible.
As the first in the UK, it is hoped that Aditi’s treatment success will lead to further investigations in the UK on how bone marrow transplant followed by a kidney transplant from the same living donor could be used to treat more seriously ill children and adults with kidney failure and other conditions. However, this will only be for seriously ill patients who have no other alternative, as the risks associated with a double transplant are greater than that of a regular kidney transplant.
Although higher risks than a regular transplant because of the bone marrow transplant, the dual transplant procedure has had good outcomes in children with Schimke’s immuno-osseous dysplasia in France, Germany and America.
Dr Giovanna Lucchini, BMT Consultant and Dr Austen Worth, Immunology Consultant, said:
"The Bone Marrow Transplant and Immunology teams worked with Aditi and her family for over a year to prepare for the dual transplant. The procedure required unprecedented collaboration between the BMT, Immunology, PICU and Renal teams. The teams had to use all their expertise and some out-of-the-box thinking to sort the scientific, ethical and practical challenges that the case presented. We are absolutely delighted to see how well she is doing, and are incredibly proud to share this success with Aditi and her family. We are already working to see how this breakthrough can underpin further research to help more families.”
Professor Stephen Marks, Clinical Lead for Renal Transplantation at GOSH and Professor of Paediatric Nephrology and Transplantation at University College London Great Ormond Street Institute of Child Health said: “This is the first time I have cared for someone in 25 years who has not required immunosuppression after kidney transplantation.
“We hope that our research will provide the option for more children, like Aditi, for whom kidney transplant was not previously an option, to have the opportunity to have a life-changing kidney transplant.”
The largest centre for paediatric kidney transplantation and stem cell transplantation in the UK
GOSH is the largest centre for paediatric kidney transplantation and stem cell transplantation in the UK, but also leads on research projects in the field.
The renal team, led by Professor Marks and funded by National Institute for Health and Care Research and Kidney Research UK, is at the forefront of testing for signs of kidney rejection after transplantation, before it happens. They are investigating the use of biomarkers which could detect a problem, before routine tests can. They hope this will mean children can be treated earlier, and with greater success.
The stem cell transplant team, led by Professor Persis Amrolia, have extensive experience in delivering bone marrow transplants to patients with incredibly complex health care conditions. They also conduct research to help improve the safety and reduce the toxicity of stem cell transplants.